The levels of troponin I and C-reactive protein improved promptly following the administration of glucocorticoid therapy. 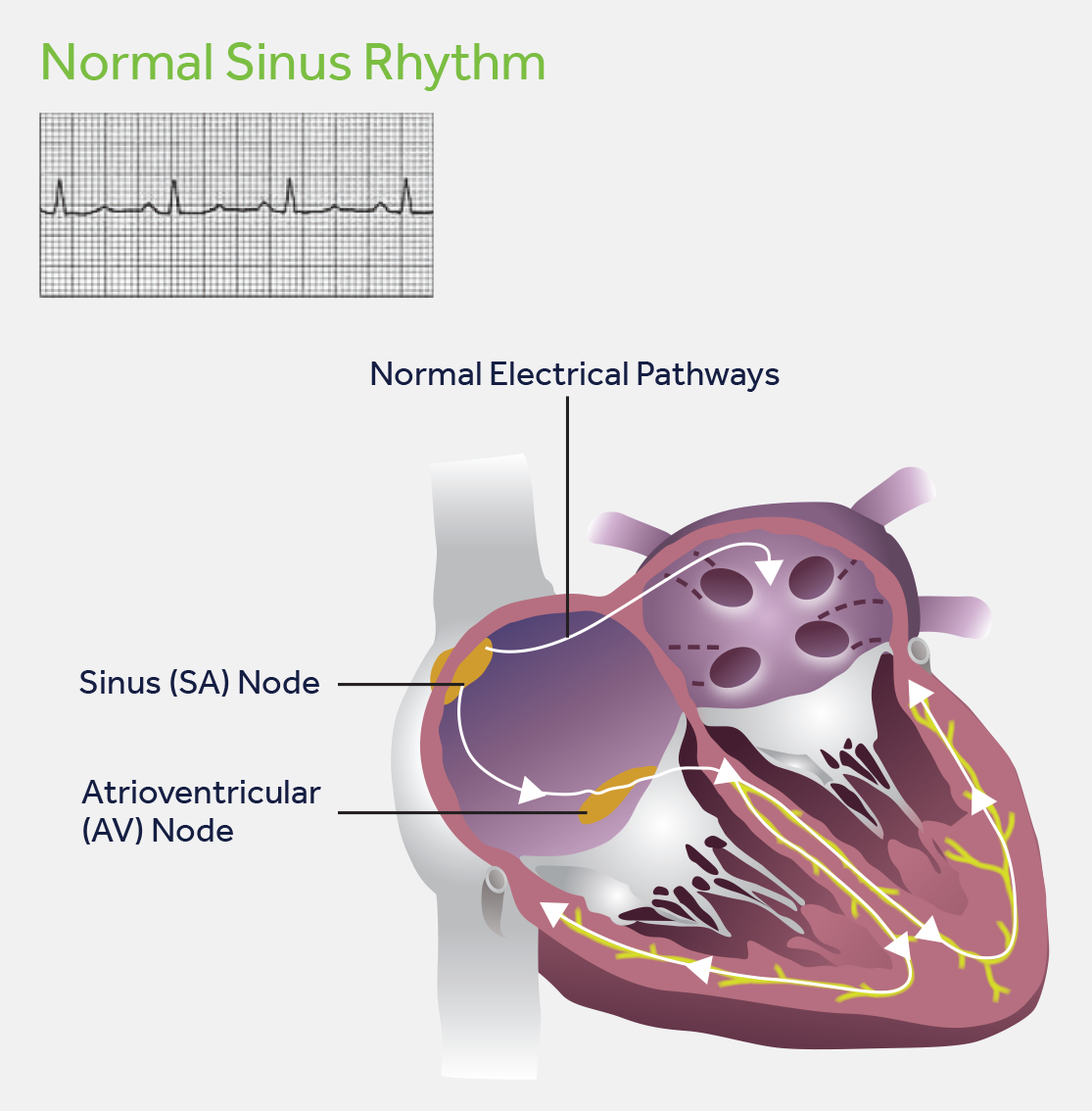
Several antiarrhythmic drugs, including amiodarone, disopyramide, carvedilol, and bisoprolol, were unable to reduce or eliminate the episodes of atrial fibrillation and repeated sinus pauses.Ĭlinical course during admission. Furthermore, de novo paroxysmal atrial fibrillation was frequently observed, combined with symptomatic sinus pauses (>5 seconds) at the termination of paroxysmal atrial fibrillation. The serum brain natriuretic peptide level was further elevated at 994 pg/dL on day 9 ( Fig. Because the left ventricular afterload had not increased, but instead had decreased, and the patient’s fluid status did not indicate volume retention as revealed by transthoracic echocardiography (the inferior caval vein was not distended, but instead had somewhat collapsed), acute left heart failure due to mitral regurgitation could not be controlled with conventional regimens, including several diuretics. With the tentative diagnosis of congestive heart failure secondary to mitral regurgitation, she was transferred to the intensive care unit. Emergent coronary angiography revealed no significant stenosis. The left ventricular ejection fraction (65%) remained normal without asynergy. Left atrial dilation, augmentation of E-wave velocity, and the appearance of an L-wave were also detected ( Fig. No echocardiographic findings indicating mitral valvar degeneration, prolapse, ruptured chordae tendineae, tethering, and papillary muscle dysfunction were observed. 3), which had been mild on a previous reading 5 months before admission. Transthoracic echocardiography showed severe mitral regurgitation ( Fig. The electrocardiogram indicated normal sinus rhythm with ST-segment depression in leads V 4-V 6 ( Fig. Chest radiography revealed cardiomegaly and congestion ( Fig. The serum brain natriuretic peptide level was elevated at 660 pg/dL. Both inflammatory markers and cardiac enzymes were elevated ( Table 1). 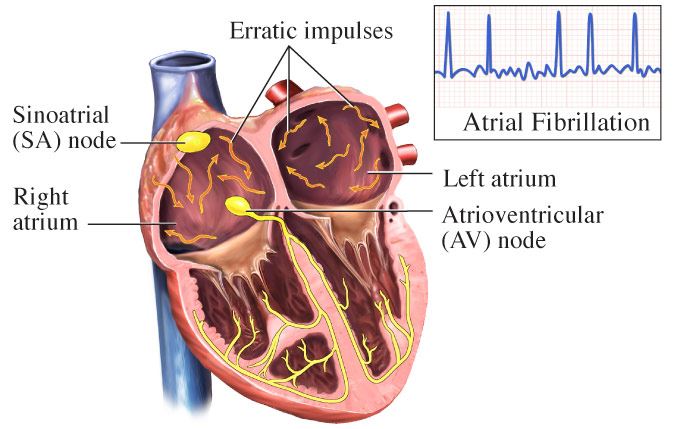
She showed a z-deformity, buttonhole deformity, bilateral ulnar deviation of the fingers, rheumatoid nodules on the lower arms, skin ulcers on the small toes, and pitting edema of the lower limbs. A prominent Levine grade II/VI systolic regurgitant murmur was audible at the cardiac apex along with a third heart sound. On admission, she was afebrile, and her blood pressure was 106/42 mmHg, with a regular pulse rate of 72 beats/min. Her past history included angina pectoris, hypertension, dyslipidemia, hyperuricemia, and bronchial asthma. She had been treated with bucillamine and tocilizumab for the last 3 years. An 80-year-old woman with rheumatoid arthritis, which had been diagnosed at 57 years of age, presented with chest pain. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
